Infertility can feel like a lonely and stressful journey for many couples. If you’ve been trying to conceive without success, you’re not alone. The good news is that modern types of fertility treatments offer multiple pathways, and understanding your options can help reduce anxiety and guide your decisions. Let’s break this down simply, step by step.
What is Fertility?
Fertility refers to the ability to conceive and carry a pregnancy. While many people think it’s just about the woman’s health, fertility involves both partners.
- Female fertility depends on ovulation, healthy fallopian tubes, and a receptive uterus.
- Male fertility depends on sperm count, motility (movement), and overall sperm health.
You might be wondering: “Does age really matter?” Yes. Female fertility often starts to decline after 30, and male fertility can also gradually reduce after 40. But there are still options at every age—knowing the fertility treatment process can help you make informed decisions.
Infertility Treatments: What You Should Know
Infertility can feel overwhelming, and many couples worry if they’ll ever conceive. Let’s break down the main types of fertility treatments for women, men, and both partners in a simple, practical way.
Treatments for Women
3D Hysterolaparoscopy
- This is a minimally invasive procedure that looks at the uterus, fallopian tubes, and ovaries.
- It helps doctors find issues like blockages, fibroids, or scar tissue.
- You might be wondering: “Is it painful?” Most patients get mild discomfort and recover quickly.
In Vitro Fertilization (IVF)
- Eggs are fertilized with sperm outside the body, then placed back in the uterus.
- Often recommended when natural conception isn’t happening despite other treatments.
- Success depends on age, egg quality, and other health factors.
Intracytoplasmic Sperm Injection (ICSI)
- A single sperm is directly injected into an egg.
- Useful when fertilization is difficult or male infertility is a factor. This is also referred to as ICSI fertility treatment, often used when traditional IVF may not be sufficient.
- This can cause anxiety, but the procedure is usually safe and done under careful lab monitoring.
Blastocyst Transfer
- Embryos are grown for five days before transfer, which may improve implantation chances.
- Doctors often use this method when multiple IVF cycles are planned.
Embryo Transfer
- The fertilized embryo is gently placed in the uterus.
- It’s a simple, short procedure done under light sedation.
Laser Assisted Hatching (LAH)
- Helps embryos “hatch” and attach to the uterus more easily.
- Often used for older women or repeated IVF failures.
Donor Programmes
- Donor eggs are used when a woman’s eggs are not viable.
- Provides a chance for pregnancy while maintaining a natural IVF process.
Surrogacy Programme
- The embryo is implanted in a surrogate mother.
- Considered when carrying a pregnancy isn’t possible for medical reasons.
You might be wondering about fertility treatment cost—it varies based on the type of treatment and clinic. Discussing this upfront with your specialist helps plan the process comfortably.
Treatments for Men
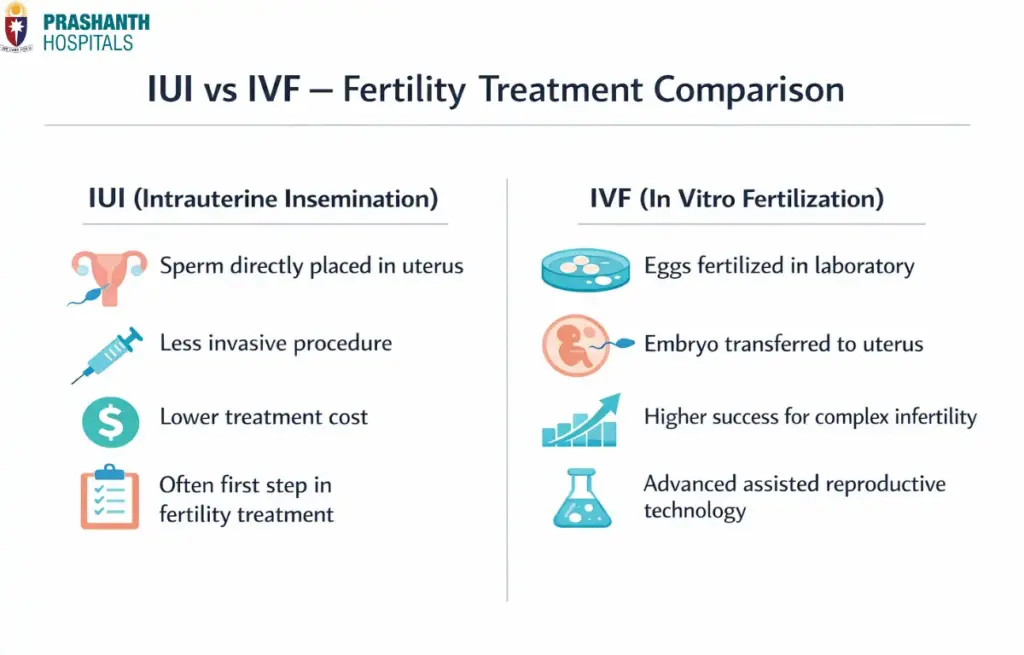
Intrauterine Insemination (IUI)
- Sperm is prepared and placed directly in the uterus to increase chances of fertilization.
- Often recommended for mild male infertility or unexplained infertility.
Intracytoplasmic Sperm Injection (ICSI)
- Used when sperm quality or count is very low.
- A single sperm is injected into the egg for fertilization. This is another example of ICSI fertility treatment used specifically for male factor infertility.
Sperm Cryopreservation
- Sperm is frozen for future use.
- Useful before surgeries, medical treatments, or if planning delayed parenthood.
Treatments for Both Partners
Hi-Tech IVF / New Techniques
- Advanced protocols are available for couples with complex infertility issues.
- Can improve success rates in specific conditions, though results may vary.
Embryo Cryopreservation
- Embryos are frozen for later use.
- Helpful if multiple IVF cycles are planned or for delaying pregnancy
Understanding the overall fertility treatment process—from evaluation to treatment—can help reduce stress and improve preparedness..
Tests for Men and Women
When couples face difficulty conceiving, doctors usually start with tests to identify possible issues.
For Women
- Hormone Tests – Measure levels like FSH, LH, and AMH to assess ovarian function.
- Ultrasound – Checks the uterus and ovaries for fibroids, cysts, or structural issues.
- Hysterosalpingography (HSG) – An X-ray procedure to see if fallopian tubes are blocked.
- 3D Hysterolaparoscopy – A minimally invasive procedure to examine the uterus, tubes, and ovaries.
Many patients ask: “Is this painful?” Most tests are minimally uncomfortable, and your doctor can guide you through pain management.
For Men
- Semen Analysis – Checks sperm count, motility, and shape.
- Hormone Tests – Measure testosterone and other key hormones affecting fertility.
- Sperm DNA Fragmentation Test – Evaluates sperm quality for more advanced cases.
If you’re worried about test results, remember that abnormalities don’t always mean conception is impossible—types of fertility treatments can often help.
Complications of Fertility Treatments
While modern fertility treatments are generally safe, they can have side effects or complications:
- Ovarian Hyperstimulation Syndrome (OHSS) – Rare, occurs when ovaries react strongly to fertility medications. Symptoms include bloating, mild pain, and nausea.
- Multiple Pregnancies – IVF can increase the chances of twins or triplets.
- Emotional Stress – Fertility treatment can be mentally and emotionally challenging.
You might also want to discuss fertility treatment cost before starting, as this helps in planning both medically and financially.
Tips for Choosing the Right Fertility Treatment
- Understand Your Diagnosis – Ask your doctor to explain test results in simple terms.
- Consider Your Age and Health – Fertility treatments work differently depending on age and underlying conditions.
- Evaluate Success Rates and Risks – Discuss realistic expectations and potential complications.
- Check the Clinic’s Expertise – Look for experienced specialists who offer personalized care.
- Plan for Emotional Support – Fertility journeys can be emotionally taxing; counseling or support groups can help.
You might ask: “Can lifestyle changes improve outcomes?” Yes, maintaining a healthy weight, balanced diet, quitting smoking, and limiting alcohol can support fertility alongside medical treatment.
Factors Affecting Success Rates
Several factors can influence how successful types of fertility treatments may be:
- Age – Younger women often have higher success rates with IVF and related procedures.
- Underlying Health Conditions – Conditions like PCOS, endometriosis, or low sperm count can affect outcomes.
- Egg and Sperm Quality – High-quality eggs and sperm increase chances of fertilization and healthy pregnancy.
- Lifestyle Factors – Stress, smoking, and diet can impact fertility.
- Treatment Protocols – Individualized treatment plans often yield better results than standard approaches.
It’s natural to feel anxious about success rates, but remember that each case is unique. Your fertility specialist will tailor the fertility treatment process to your situation.
Conclusion
Fertility challenges can be stressful, but understanding the process helps reduce uncertainty. From tests to types of fertility treatments, options are available for women, men, and couples together. While no treatment guarantees pregnancy, modern medical advances provide multiple pathways to support conception safely.
If you’re worried about infertility, the first step is a thorough evaluation with a qualified fertility specialist. Even small steps—like understanding your test results or lifestyle adjustments—can make a significant difference.




